Meniscus
The meniscus is avascular structure within the knee. There are two of them in each knee on the medial (inside) and lateral (outside) of the knee. They are c-shaped and have no direct blood supply. They derive their nutrition from the fluid in the knee and from blood seeping in from the peripheries of the meniscus. They function as shock absorbers within the knees and essentially the “cushions” in the knee. The menisci are therefore extremely important in preserving the longevity of the knee.

The problem when one injures the meniscus, is that it does not heal itself as it has no blood supply. For this reason, most meniscal surgeries involve removing the torn piece. This is not entirely correct though and the meniscus does have the potential to heal in the correct conditions, when it receives a blood supply. The meniscus is there for a reason and an attempt should be made, where possible, to save the meniscus and repair it.
TREATMENT OPTIONS:
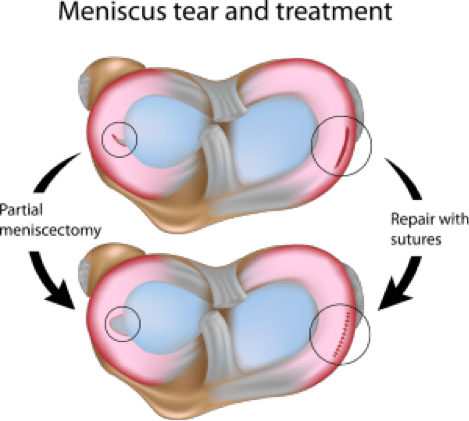
- Partial meniscectomy – the torn part of the meniscus is debrided and removed back to stable meniscus. This stops the tear from propagating and flapping into the joint and alleviates the pain and discomfort. Unfortunately this is what is done in the majority of cases. Recovery is quick with no brace and return to full activities in 2-4 weeks.
- Meniscal repair – the tear is stitched back together in order to try and facilitate healing. The recovery from this procedure is significantly longer with the repair being protected in a brace for 6 weeks and then protected activity allowed for a further 6 weeks.
HOW DOES THE REPAIR WORK AND HEAL?
At the time of arthroscopy, if the surgeon decides that the tear is repairable (most tears are irreparable), he will go ahead and suture the torn meniscus. We then try to stimulate blood to seep into the repair and aid healing. This is done by making “vascular channels” in the surrounding soft tissue within the knee. This then causes blood to ooze into the repair.
Another means of aiding the healing is to release stem cells into the knee. This is done by making small holes in the bone within the knee, in an area that is unimportant and not a weight bearing area. The area most commonly used is the notch of the femur. This allows stem cells to ooze out of the bone and into the knee, where the stem cells can reach the repaired area and aid healing.
All these methods are attempting to get blood and growth hormones in the blood, to the area of healing and hopefully end up with a successful repair. Even with all the methods attempted to aid the healing, not all repaired meniscus heals and about 20% fail and the tear never heals. Eventually when the sutures fail, the torn piece of meniscus comes loose again and necessitates and second operation in order to remove the torn piece of meniscus.
MENISCAL TRANSPLANT
Unfortunately in some the whole meniscus is defunctioned or been removed in previous surgery. This leads to increased contact area and stress of the articular cartilage and is well known to accelerate degeneration in the knee leading to osteoarthritis.
In these cases, options are limited and a meniscal transplant may be recommended to alleviate symptoms and hopefully prevent or decrease the chance of osteoarthritis. There are two possibilities for meniscal transplants. Fresh frozen allograft from an organ donor, where the meniscus is sized to match your meniscus which was removed. These fresh frozen allografts are currently being sourced from Belgium as unfortunately the meniscal allografts in South Africa are irradiated, significantly decreasing their strength. These fresh frozen allografts give the best results.
The other option is a meniscal scaffold or synthetic meniscus. These rely on tissue growing into the meniscal scaffold. The results of these are less predictable.
I perform all the above surgeries and individualise the procedure to each patient and their best interests.